The story of Archie du Preez

The day Archie was born, we were told “This is the worst case we have ever seen”, “I haven’t seen anything quite like this in my career”, “I don’t know what is wrong with his lungs”.
Being told your newborn baby, in our case, twin 2, is unwell and may not survive the next 48 hours is not something any parent wants to hear.
We were petrified. We were scared of losing our baby. Our boys were born prematurely at 30+4 at the Mater Mothers Hospital, Brisbane. The story leading up to this moment can be found by clicking here.
Archie’s initial diagnosis
Within 40 seconds of birth, Archie had respiratory failure and was intubated. It was clear to the doctors, at that moment, that something was catestrophically wrong with our tiny baby.

Weighing in at 1.23kg (2.7lb), Archie was born with Chronic Neonatal Lung Disease, Interstitial Lung Disease, Patent Ductus Arteriosus (PDA), Pneumonia and Jaundice.
The doctors were so unsure what was wrong with Archie, they had to start treating him blindly, hoping something would help him. Archie had several blood gases, full blood workups, multiple chest and abdomen X-rays, echocardiograms, head ultrasounds, blood cultures and Retinopathy of prematurity (ROP) eye testing (which is a disease of premature babies that causes abnormal blood vessels to grow in the retina, the layer of nerve tissue in the eye that enables us to see. This growth can cause the retina to detach from the back of the eye, leading to blindness) all within the first few days.
They started Archie on antibiotics to see if that would clear the Pneumonia, which could be causing the fluid in his lungs. They also started him on Ibuprofen which is the first step to treating the PDA and getting this to close, which in most babies happens naturally after birth. Archie had two rounds of ibuprofen (6 August and 9 August and a round of paracetamol which started on 13 August).
What is a PDA?
In PDA, abnormal blood flow occurs between two of the major arteries connected to the heart. Before birth, the two major arteries-the aortae and the pulmonary artery-are connected by a blood vessel called the ductus arteriosus. This vessel is an essential part of fetal blood circulation.
Our Doctor thought that the PDA may be a contributing factor for the fluid, so if that was treated, it may help identify the underlying lung issue. Thankfully the PDA closed on 16 August and did not require surgery – yay! But, this did not help Archie’s lungs so we were back to the drawing board.

We think it’s something extremely rare…
The doctors started talking about all of these medical terms and possible diagnosis which meant nothing to us at the time. So, we asked a lot of questions and Steven did a lot of research, something I didn’t want to do because the results of these specific tests, if positive, was something we did not want for our baby. They all resulted in some serious disability or even death.
Two days after birth, Archie was tested for the Surfactant Protein DNA as the specialists thought he may not be producing the surfactant. Thankfully this test came back negative, but also meant we were back to the drawing board… again.
An Endotracheal tube (ETT)Lavage was also done two days after birth to get a sample of the fluid to be sent off to the lab to determine what exactly this disease could be.
It was a never-ending guessing game, with our Doctor sending off just about every test imaginable. This at one point included testing for the NKX2-1 variant which required blood samples from both Steven and myself to check for a genetic disease, this was also negative.
Respiratory Support from birth
Archie was intubated at birth which means he was put onto a high-frequency ventilator which essentially gave him around 300 breaths per minute. Without this type of ventilator, Archie’s lungs would have collapsed.
I had my first kangaroo cuddle 9 days after Archie was born whilst Archie was on the high-frequency ventilator. It was the most stressful cuddle of my life. I had to hold the back of Archie’s head firmly because if he pulled back and the tube came out, he would be in serious trouble. I was petrified that I was going to move and pull the tubes out.

On 16 August 2018, at 10 days old, Archie was put onto a conventional ventilator. This was only for 4 days when the team decided to try Archie on CPAP (Continuous Positive Airway Pressure), and he surprised everyone and managed well.

Archie hated CPAP, he would manage to face plant in the right spot to disconnect the snorkel on his face, which of course caused him to desaturate! He absolutely kept the nurses busy 🙂
With one failed attempt, on 5 September 2018, on high flow, Archie finally transferred over to High Flow on 19 September 2018. He found this to be much more comfortable.

We could finally look at his beautiful little face without a giant plastic snorkel on. This is when we started to get some smiles from our little man. He was finally able to feel like himself. His smile was contageous.
For Archie, every day he had to fight, fight for his life. This is something we didn’t ever forget. He would go from being good to desaturating in an instant.
Imagine running a marathon, only you’re unable to stop for a break and catch your breath. This is how Archie felt every day. He was running a marathon.
It’s now time to start Steroids
The words we didn’t want to hear. It was a last resort. We were once told that steroids are poison and we will avoid giving them for as long as practically possible. So, when our Doctor said we need to start a round of steroids, we felt sick. The list of side effects of giving doses of steroids particularly to a premature infant is long… very long. They told us it could potentially cause a neurological disability, it could cause developmental delays amongst many other things.
We had no choice. This was the best course of treatment for giving Archie any hope of survival. Archie’s first dose of Dexamethasone (Dex) was given on 23 September followed by another dose on 11 October.
Roid Rage is a real thing, even in neonatal babies. There were a few days in each course that made Archie angry and frustrated. But, we took every opportunity to make sure Henry and Archie had plenty of play time!


Our Doctor wanted to try a course of Methylprednisolone (Methyl Pred) which is a 3-day course of steroids. This didn’t make a difference for Archie so it was back to the Dex after that.
1 in 3 chance of survival…
We met with Archie’s respiratory specialist, who was an absolutely incredible Doctor. He was very honest with us, right from the beginning, which we really appreciated.
He told us he hasn’t seen anything quite like this before and was unsure what the actual diagnosis was. We were told that a Lung Biopsy and Bronchoscopy were the last remaining steps in attempting to diagnose the underlying lung disease. Even with these procedures, there is a chance that no diagnosis would be determined. However, they could work out if there is treatment suitable or not.
We were also advised that a baby has significant growth in the 3 – 6 month period and this is where we would likely know if Archie’s lungs were going to manage. Our Respiratory Doctor said that we will know by the time Archie reaches 6 months if his lungs will manage with his growth or not. For us, 6 months would have taken us through to February 2019.
A 1 in 3 chance of survival is what we were told we were dealing with. As a parent, hearing those odds and knowing your Doctor is more pessimistic than optimistic is very hard to hear. However, our Doctors never ever gave up.
100 days in NICU… well 95 days!
When your baby hits 100 days in the NICU, there is a party! Archie was transferred to Queensland Children’s Hospital at 95 days so the wonderful team arranged an early 100-day party for Archie. It was so sweet.

It’s time to leave NICU and head to PICU
Something we didn’t want to happen. We didn’t want to leave our amazing Neonatologist, the wonderful nurses who had become our friends. We didn’t want to have to start again. However, we kept the same Respiratory specialist which we were really happy with as he has worked so hard for Archie in the first 95 days.
Although we didn’t want to go to Queensland Children’s Hospital (QCH), we understood the reason why. Archie had become a term baby and his requirements and development needs were something that QCH could offer Archie.
It’s time for a Lung Biopsy and Bronchoscopy…
The last thing on the list… a Lung Biopsy and Bronchoscopy… We weren’t sure if it was something we wanted to do. It wouldn’t change the outcome, so why put him through surgery and being ventilated again?
The answer was simple in the end. The simple truth was that the biopsy could possibly determine the disease but more importantly for us, it could possibly determine if there is a treatment plan or not.
We made it clear from the very beginning to the Doctors that we only ever wanted what was best for Archie and doing procedures unnecessarily was something we weren’t interested in. We also didn’t want to continue to pump steroids into his tiny body, for what could be absolutely no reason at all. So, we decided to go ahead with the Lung Biopsy. For this, we had to wait until Archie had reached 3.5kg in weight.

At this point in time, it was the hardest thing I had to do as a mum… walk my baby down to the operating rooms and leave him there to be ventilated again in preparation for surgery. I lay him down on the bed and the doctor had accidentally removed his feeding tube while repositioning his tape on his face. Archie was distraught. The doctor looked at me and asked me to leave. It was one of the hardest moments of my life, leaving him there so upset.
The whole procedure took a couple of hours and they wheeled him back up to PICU, still ventilated and sedated. It was so hard to see him like that, with all the tubes, drips and machinery… it took me back to when he was first born.


The results of the biopsy and bronchoscopy
We waited a very long week to hear anything back. We sat down with the respiratory consultant who was working that week, the same Doctor who had arranged Archie’s biopsy and bronc, and she showed us a series of images. She was showing us the images of Archie’s lungs and explaining to us the tissue we were seeing was not good tissue. We asked her to show us what a good piece of lung tissue looked like… she spent a few minutes and then said, “I’m sorry, I can’t see any good lung tissue”. It was at that moment, I realised that there was little to no hope for our little warrior.
What they did see is that there was an Alveolar Growth Abnormality and Alveolar Growth Simplification.
Alveoli are an important part of the respiratory system whose function it is to exchange oxygen and carbon dioxide molecules to and from the bloodstream. These tiny, balloon-shaped air sacs sit at the very end of the respiratory tree and are arranged in clusters throughout the lungs.
For this, there is no treatment. No steroids, no medication, nothing. We sit and wait, we wait for Archie to grow and see if his lungs grow with him and support his weight growth and development.
Off to the babies ward, 9B
We transferred from PICU to the Babies Ward which we were so happy about. We didn’t have the best experience in PICU so being in the babies ward was a good move for us. The nursing staff in the babies ward were fantastic and because they choose to work with babies under the age of 1, their care for the babies is wonderful – they wanted to be there.
We were doing so well. Archie was enjoying Music Therapy with Maggie twice a week – a highlight for all of us there. We had regular visits with Physio, Occupational Therapy and Speech Therapy. Archie was developing really well. He was doing everything we wanted him to do. He was such a clever boy!
We had a glimmer of hope…
He was growing but at this
But our glimmer of hope was short lived when Archie developed Bronchiolitis.
I had put Archie in his swing in the cot and he was watching some TV. He was calm and peaceful… next thing I hear the alarms ringing and his heart rate sitting at 210, I thought this can’t be right… he isn’t upset, the sats probe on his foot must be falling off. I checked it, it was fine, Archie wasn’t upset, but I noticed he was sweating a lot. I called the nurse over and she did a quick set of obs and very quickly realised that it was accurate and something wasn’t quite right.
The Doctors were sure he had picked up Bronchiolitis and we were moved to an isolation room and a course of antibiotics was started to try and treat this infection. We spent nearly two weeks with Archie fighting this infection. Every day Archie gave us smiles, he was such a happy baby despite what was going on.

Our first family Christmas
Something we thought we would never get as a family of four… our First Christmas.
The festive season started for us when two amazing nurses, Billy-Jo and Rosie, arranged a portable high flow from PICU and helped us go down to see Santa for the boys first Santa photo.


It was so nice to leave Archie’s room, even it was for such a short time! We went down for our Santa photos and then on the way back up, we went onto the balcony for a half hour and enjoyed the fresh air and wind in Archie’s long hair. It was such a beautiful afternoon.
On Christmas morning, we arrived to see a drip in Archie’s arm. He had a very high temp overnight and struggling to fight it and seemed quite unsettled and unwell. Definitely not how we wanted to spend Christmas Day, or any day to be honest. But, it is what it is and we had to make the most of the time with our boys.

The incredible staff had made onesies for both the boys, a gorgeous frame and presents for not just Archie, but for Henry as well. It was a really special day and it didn’t matter that we were in the hospital, we were all together and that was the main thing.

Then, it all started to feel wrong…
Call it mother’s intuition if you like, but on Monday morning, the 7th of January 2019, I knew something wasn’t right with Archie.
I spent the day holding him, like every other day. He was working hard. So hard. To do something as simple as a fart, he struggled… it took every ounce of energy he had to get it out. He would desaturate and then require an increase of oxygen to get him back up again. Then, when he had to do a poo, it was traumatic, for both of us. He would get so upset, he would sweat, balls of sweat on his head, again the oxygen had to be increased just to get him back up to where he needed to be.
It was a struggle. I went home and said to Steven that something wasn’t right. On Tuesday morning, the Doctors doing the rounds said that our respiratory Doctor wanted to meet with us on Thursday. I knew right away what they were going to tell us. At this point, I was scared. I was scared of what he was going to tell us. It was the longest few days.
The meeting that changed our lives…
We met with the Doctors on Thursday afternoon. It was a conversation I had imagined over and over in my head… I thought I was prepared for what he was going to tell us. I wasn’t. Nothing can prepare you for your Doctor telling you that your baby is struggling. His liver had started to compensate, his increased oxygen requirements a few weeks prior indicated that he was struggling to cope with his increased weight and development.
It was at this point, our Doctor wanted to meet again the following Tuesday to talk about the next steps and getting the Palliative Care team involved.
Just hearing the words Palliative Care… I knew it was the beginning of the end.
Archie’s high flow requirements had increased from 9L to 10L and his Oxygen is averaging around 40%. There was a point that Archie’s oxygen was room air (21%). Archie’s C02 output had increased to around 70. The Doctors started a 3-day course of Methylprednisolone to try and help Archie feel a little better. It was an attempt to let Archie know that we hear him and are trying to make him more comfortable.
On Friday morning, our Doctor wanted to meet again and bring forward the Tuesday meeting. They explained to us the reason why Archie was starting to work a little harder. This is due to the fact that Archie has set a new baseline for his C02. His body has started to help him manage this new baseline, but as a result, his other organs are starting to help. When Archie is desaturating, he becomes hypoxic (lack of oxygen flowing through the blood) which makes him very unsettled and uncomfortable.
The Babies Ward we were in bent all sorts of rules to accommodate us so we didn’t have to go back down to PICU and would allow Archie to stay in the ward until his flow hits 3L per kilo (around a flow of 15) and his oxygen hits 50%. If Archie had required additional support to this, he would have been moved down to PICU.
Although we see Archie’s doctors daily, we sat down in a family meeting to have a very real and honest conversation about Archie’s current state. This is the meeting we were told Archie will start another 3 days of steroids. The steroids were not a treatment for what Archie has (there is no treatment), which is Chronic Neonatal Lung Disease, Interstitial (Unknown) Lung Disease with an Alveolar Growth Abnormality. However, the steroids would hopefully let Archie know we hear that he is uncomfortable and this will provide some comfort to him and he will know we are trying to help ease this for him.
In the meeting on Friday afternoon, Archie’s Doctors asked me to sign a DNR (do not resuscitate) form. This is for if Archie’s saturations drop to a level where he is transferred to PICU and they will attempt to ventilate Archie and if he flatlines will provide CPR, which is not what we wanted them to do for Archie. This form ensured Archie would not end up on a ventilator.
We knew at this time, Archie was in his final weeks of his life…
Our Doctors referred us to Palliative Care and their job was to help manage Archie’s pain with medication to ensure he was comfortable and doesn’t have periods of unsettledness. Steven and I spent every day with our little superhero, making memories that will last us a lifetime. Archie fought so hard to get to this point. Considering we were told he wouldn’t survive 48 hours, let alone a week or two to make it past 5 months of age. He was a true Miracle and an absolute superhero. We were so lucky to be able to get to know him.

The incredible Palliative Care team…
I can’t speak highly enough of this wonderful team. The work they do is outstanding. We met with the team over the weekend. They asked us one question… “What is the one thing we can do for you?”
The answer was simple, but we thought was out of reach… We said we would like to bring Archie home. Without hesitation, they said they will start working on it and do everything they can to make it happen.
We asked for one other thing.. that was to spend Archie’s end of life at Hummingbird House. They started working on logistics on how that might work as well.
Archie’s Great Adventure – Day 162
Archie’s Great Adventure, named by Karen in the Palliative Care Team, was in full swing. It was happening. We couldn’t believe we were taking our baby home, finally.
Logistically, it was very difficult to arrange. Firstly, they had to arrange the Queensland Ambulance Service and retrieval team to agree to help with the transfer to and from the hospital. Then a portable high flow and oxygen had to be sourced not only for the transfer to and from but also for our apartment. Nothing about this was simple. We weren’t even sure how Archie would cope with the transfer.
The morning arrived… this was it. It was Wednesday, 16 January 2019, we arrived at the hospital, only to find that our wonderful nurse, Vanessa, had made onesies that said Archie’s Great Adventure and also ones that had the boys names on them. It was amazing.
Steven and Henry waited at home and I came via Ambulance with Archie.
From the moment we got to the ambulance from the hospital room, Archie was distressed. I thought right away that they would call the whole thing off and we wouldn’t get our day at home. The staff gave Archie some additional medication to help calm him down and I gave him some sucrose with his dummy. Thankfully, after a few minutes, it did the trick and he slept the whole way home.
Part 1 of the journey started with an ambulance ride from QCH to home. We were able to take Archie to his room, he had a play in his cot and the moment he was put in the cot, the smiles were there. He was so happy to be at home.


From there we moved into the lounge room. Archie had a lovely time playing chimes with his brother, laying under his activity centre and reading a very special book to Henry. Steven and I were able to spend such quality family time together, without any doctors and nurses in sight.

Thankfully, it took the ambulance crew a while to find the extra large ambulance so Steven and Henry could ride with us, so we got an extra 1.5 hours at home. We then moved into our room where Henry visits each morning and the boys had a lovely sleep.

Then, it was time for Part 2 of Archie’s Great Adventure. A trip to the Botanical Gardens. This was the most special part of the day. Henry and I walked this path well over a hundred times going to and from seeing Archie in the hospital. We always talked about how much Archie would love it in the park, watching the trees, birds and the water. To be able to show Archie these things was the most special moment we could ask for as parents.

It is safe to say that Archie had the best day of his life and so did we.
Hummingbird House… Our Final stop
Our final stop on this roller coaster of a journey.
We arrived at the hospital on Thursday, 17 January 2019.
We thought the plan was to head to Hummingbird House on Thursday, have all of our family visit on Friday and Archie would be free from his high flow on Saturday.
On Thursday morning, we found out that this wasn’t the case and Hummingbird House cannot cater a child on High Flow for more than a couple of hours.
We then had to make a decision very quickly, if we still wanted to go to Hummingbird House that day or push it out to another day.
The reality had sunk it… today was likely going to be the last day our superhero was on this earth. We knew it was coming, but nothing really prepares you for this moment, and decided to continue with our plan to go to Hummingbird House.
We rang our family to see if they could change their plans and go to Hummingbird House on Thursday afternoon. This meant my brother and his fiance changing their flights from Sydney as they were due to come on Friday morning.
We arrived at Hummingbird House and went straight out to the garden. Our family visited throughout the day to say goodbye to our little boy.

Superhero turned Angel
After a beautiful night sleeping under the stars, our little Archie decided to put on his angel wings at 4.20am on Friday, 18 January 2019.
Thank you to Hummingbird House who welcomed Archie into their home. From the moment we arrived, we ditched the indoors and spent every second outside with the trees, birds and breeze. Archie was so incredibly happy to be there, giving us plenty of smiles. The staff arranged a bed outside under the stars so we could stay outside as a family, a wish we had for Archie, to live out his final day in the fresh air and under the stars.

Our brave little boy had his high flow removed at 6.10pm on Thursday night, 17 January 2019, and we enjoyed the next 10 hours and 10 minutes wire and tube free while snuggling as a family of four under the stars. Archie grew his angel wings just as the sun came up and the birds started to chirp. We couldn’t have asked for anything more for our boy.
Archie passed away very peacefully, surrounded by his mummy, daddy and brother Henry. We made some magical memories over the 5 and a half months we have had the pleasure of knowing Archie and he made us so very proud with how bravely he fought from the moment he was born and how he defied his diagnosis at every step and even grew his wings in his own time, on his own terms. Steven and I will be forever grateful to our Doctors who never gave up and allowed Archie to determine his own path.

Archie will be missed every day for the rest of our lives. We are so grateful to have gotten to know our little superhero and the luckiest parents that he chose us to be his mummy and daddy and Henry to be his twin brother.
A farewell fit for a superhero…
We had the most beautiful service for Archie. It was unique and everything we could have hoped for. Click here to read more about our farewell.




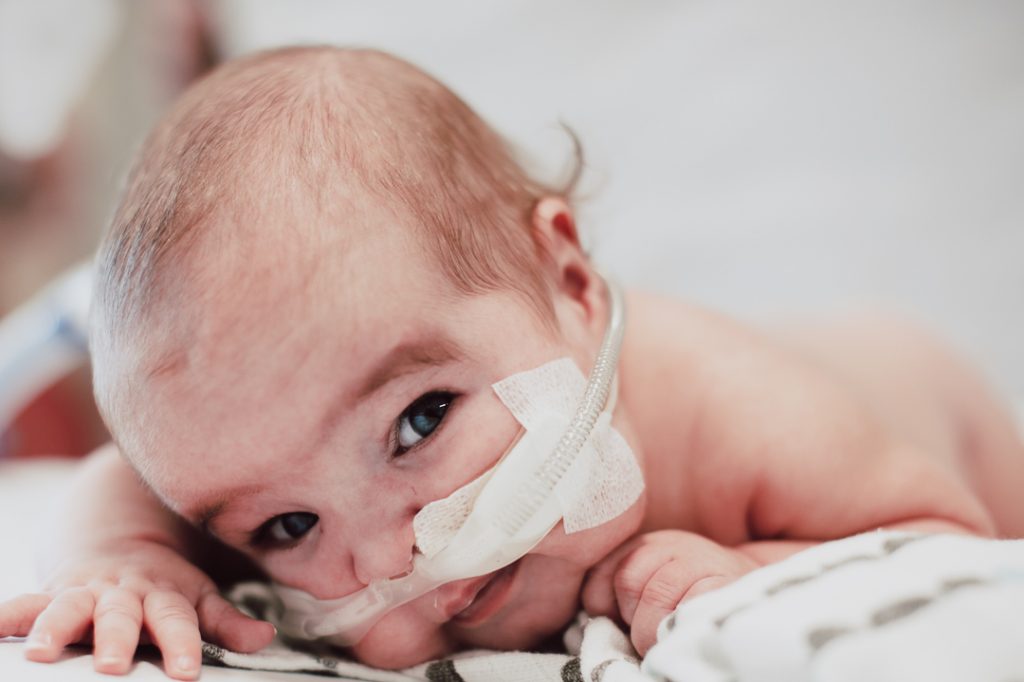


Fly high our superhero angel.
You will forever be in our hearts.

Pingback: A farewell fit for a superhero - The Well Travelled Family
Wow, you all are so wonderfully brave. Archie was a handsome little fellow, and such a trooper. Beautifully written story of your time together with your son. xo
Thank you Tamie for your kind words. He was a handsome little fellow, you’re absolutely right 🙂
Pingback: 15 Gift Ideas for Parents with babies in NICU - The Well Travelled Family
Omg I just read this tears in my eyes. I can’t even begin to imagine how hard this would have been for you guys. So much love and support for you all xx
Thank you for reading Casey x